Numbness, back pain, or leg heaviness slowing you down? It could be Spinal Stenosis or Spinal Atrophy. You can feel better without guesswork. Learn the fastest, safest paths to lasting relief.
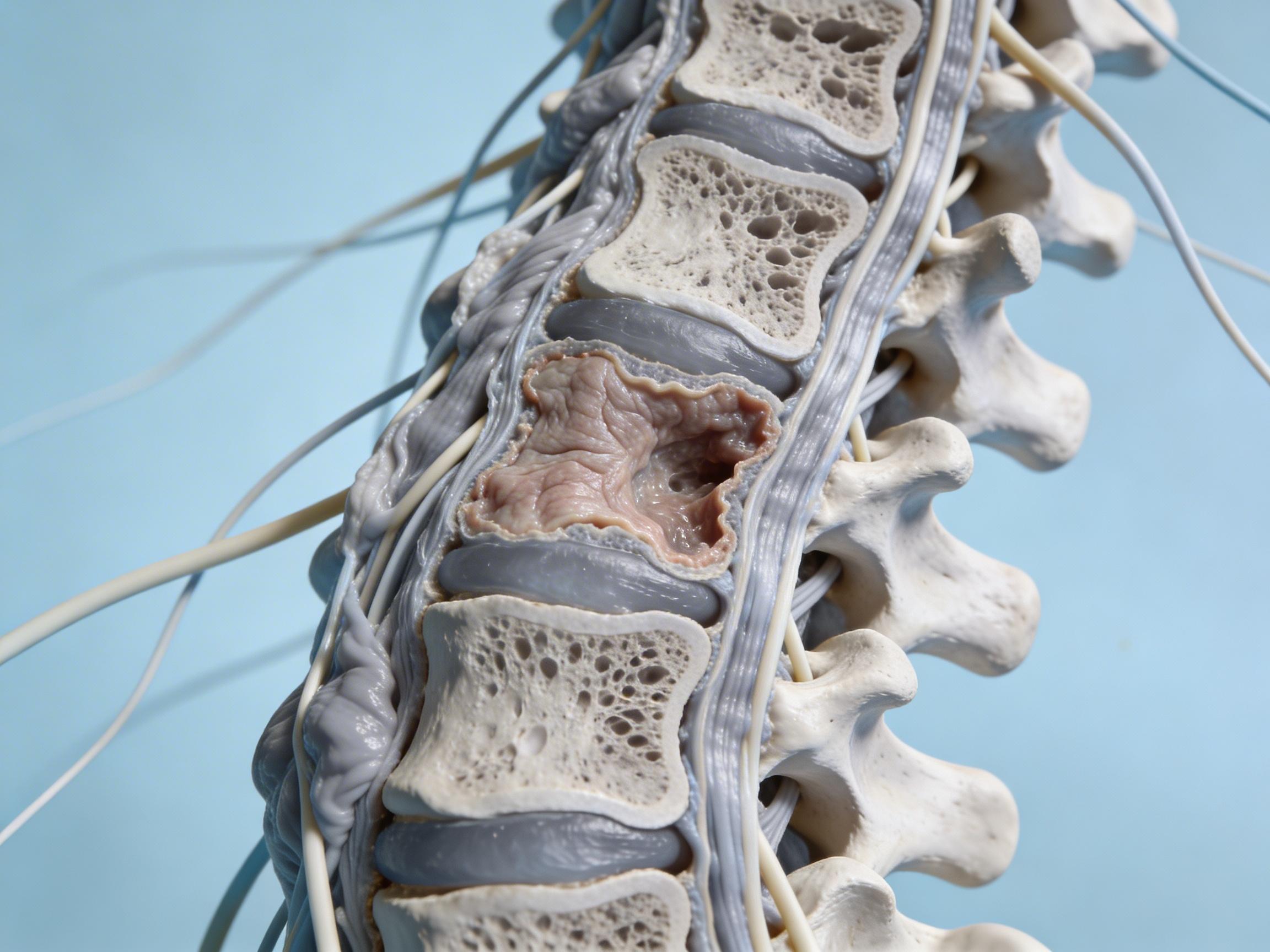
What Is Spinal Stenosis?
Spinal stenosis is a narrowing of spaces in your spine that crowds nerves. It most often affects the lumbar (lower back) or cervical (neck) regions and can cause back pain, tingling, burning, or weakness down the legs or arms. A hallmark of lumbar stenosis is neurogenic claudication—leg heaviness or pain that worsens with standing and walking and eases when you sit or lean forward. For a clear, patient-friendly overview of causes, symptoms, and standard care, see the Cleveland Clinic’s resource: Spinal Stenosis: What It Is, Causes, Symptoms & Treatment.
Stenosis can happen centrally (in the main canal), in the lateral recess, or at the foramina where nerves exit. Arthritis-related bone spurs, thickened ligaments, disc bulges or herniations, and vertebral slippage (spondylolisthesis) can all reduce nerve space. Cervical stenosis can also cause hand clumsiness, balance difficulties, or in severe cases, signs of spinal cord compression.
What Causes Spinal Atrophy—and How It Ties to Stenosis
When people ask “what causes spinal atrophy,” they usually mean muscle atrophy near the spine, hips, and legs that makes standing and walking harder. In the setting of stenosis, atrophy has three common drivers:
- Nerve compression–related denervation: Pinched nerves fire less effectively, leading to shrinkage of the muscles they supply. This often shows up as focal weakness or visible thinning.
- Disuse and pain avoidance: Pain and fear of symptoms make you move less, accelerating loss of muscle fibers and endurance.
- Age-related sarcopenia and inflammation: With aging, baseline muscle mass drops and inflammatory changes from arthritis amplify the decline.
Left unaddressed, atrophy can persist even if pain improves, which is why treatment should pair symptom relief with progressive strengthening. For additional background written for patients, review the American College of Rheumatology’s page: Spinal Stenosis.
Diagnosis: Getting the Right Answer
A precise diagnosis ensures you treat the true cause of pain and weakness. A clinician will take a careful history (including whether symptoms improve when bending forward), examine strength and reflexes, and rule out vascular claudication. Imaging clarifies anatomy:
- MRI: Best first test to visualize discs, ligaments, nerves, and the canal.
- CT myelogram: Useful when MRI is not possible or to clarify complex postsurgical anatomy.
- X-rays: Show alignment issues like spondylolisthesis or scoliosis that can worsen narrowing.
- EMG/nerve studies: Sometimes used to map chronic nerve injury and differentiate overlapping conditions.
For a practical overview of testing and care pathways, see Mayo Clinic’s guide: Spinal stenosis diagnosis and treatment. Brown University Health offers a succinct symptom and therapy snapshot here: Spinal Stenosis: Symptoms and Treatment.
Best Treatments for Spinal Stenosis
The most effective plan matches symptom severity, anatomy, and goals. Many people improve without surgery, while some need a targeted procedure to free compressed nerves.
- Activity modifications: Short, frequent walks; leaning forward with a walker or trekking poles; and pacing strategies reduce nerve crowding during movement.
- Physical therapy: Core and hip strengthening, flexion-biased conditioning (e.g., recumbent cycling), and nerve-mobility drills improve endurance and mechanics. Addressing gluteal and spinal extensor endurance helps reverse atrophy.
- Medications: Short courses of NSAIDs, neuropathic pain agents (like gabapentin or duloxetine), and topical analgesics can reduce pain enough to allow quality rehab.
- Epidural steroid injections: Useful for flares or when leg pain dominates, buying time for rehab. Relief can be temporary but meaningful for many.
- Facet or medial branch care: If facet arthropathy is the main driver of back pain, medial branch blocks and radiofrequency ablation can help the axial component—but they do not open the central canal.
- Minimally invasive decompression: Options include the MILD procedure (debulking thickened ligament) or interspinous spacer implants in carefully selected patients.
- Decompressive surgery: Laminectomy or laminotomy (with or without fusion if instability exists) remains the gold standard for severe neurogenic claudication or progressive neurologic deficits.
To compare options, this overview of nine approaches is a helpful read: Nine Spinal Stenosis Treatment Options to Help with Pain. The Cleveland Clinic resource above and Mayo Clinic page also summarize evidence-based choices and when to escalate care.
How to Treat Spinal Atrophy From Stenosis
Relieving nerve compression is only half the job; rebuilding muscle is essential to lasting freedom of movement.
- Progressive strengthening: Start with low-load exercises that avoid symptom provocation—such as seated marches, bridges with a posterior pelvic tilt, and supported squats—then progress to dead bug variations, hip hinges, and step-ups. Aim for 2–3 sessions per week, with gradual increases in volume.
- Conditioning in flexion-friendly positions: Recumbent cycling, treadmill walking with slight incline and forward lean, or aquatic therapy keeps nerves decompressed while boosting endurance.
- Neuromuscular activation: For focal weakness (e.g., ankle dorsiflexors), add isolated activation sets or neuromuscular electrical stimulation as guided by a therapist.
- Pain control to enable training: Timed medication or injections can create a therapeutic window to push quality repetitions safely.
- Nutrition: Adequate protein (roughly 1.0–1.2 g/kg/day unless restricted), vitamin D sufficiency, and creatine monohydrate (if appropriate) support muscle recovery.
Most people see stamina gains within 4–6 weeks and strength changes by 8–12 weeks, with continued improvements for 6–12 months.
When to Seek Urgent Care
Get immediate help if you develop new or worsening leg weakness, numbness in the saddle area, trouble starting or stopping urination, loss of bowel control, fever with severe back pain, or a fall with new neurologic symptoms. These red flags can signal severe nerve or cord compression requiring urgent evaluation.
Costs and Insurance: What to Expect
Prices vary widely based on region, facility type, and insurance. The estimates below reflect typical U.S. cash-pay ranges compiled from public self-pay schedules and national pricing tools (FAIR Health, Healthcare Bluebook, clinic disclosures) as of 2024. Always confirm your benefits and ask for a written estimate. If you live in Columbus, check local hospital transparency tools; many now publish bundled prices you can compare before scheduling.
| Service (Common for Stenosis) | City / Source | Typical Cash Price (USD) |
|---|---|---|
| Lumbar MRI (no contrast) | National Average (FAIR Health) | $450–$1,200 |
| Physical Therapy Session (60 min) | Dallas, TX (Healthcare Bluebook) | $90–$160 |
| Epidural Steroid Injection (Lumbar) | Phoenix, AZ (FAIR Health) | $700–$1,500 |
| Medial Branch Radiofrequency Ablation (2 levels, one side) | Chicago, IL (Healthcare Bluebook) | $3,000–$6,000 |
| Minimally Invasive Lumbar Decompression (MILD) | National Estimate (Facility + Professional) | $6,000–$12,000 |
| Interspinous Spacer Implant (e.g., Vertiflex/Coflex) | Los Angeles, CA (Facility + Device) | $9,000–$17,000 |
| Lumbar Laminectomy (no fusion) | New York, NY (Healthcare Bluebook) | $18,000–$38,000 |
| Laminectomy with Fusion (1–2 levels) | National Average (FAIR Health) | $55,000–$110,000 |
| Chiropractic Evaluation + Adjustment | Atlanta, GA (Cash Clinics) | $60–$120 |
| Initial Pain Management Consult | Houston, TX (Cash Pay) | $200–$350 |
| Gabapentin 300 mg, 90 capsules (generic) | National Retail (GoodRx low est.) | $9–$20 |
Note: These figures are nonbinding estimates. Your actual costs will depend on plan design, deductibles, network status, and facility fees.
A Week-One Action Plan for Relief
- Book an evaluation: See a spine-savvy primary care clinician, physiatrist, or spine surgeon for an exam and to order imaging if needed. Ask specifically whether your pattern suggests lumbar stenosis or another cause.
- Start flexion-friendly movement: Try 10–15 minutes of recumbent cycling or gentle uphill walking twice daily, stopping before sharp pain.
- Begin targeted strength work: Focus on core bracing, hip hinges with support, bridges, and step-ups every other day. Track sets and symptoms.
- Dial in pain control: If appropriate, time NSAIDs or neuropathic meds 30–60 minutes before exercise. Discuss risks and alternatives with your clinician.
- Plan follow-up options: If walking tolerance remains under a block after 6–8 weeks of consistent therapy, discuss injections or minimally invasive decompression; consider surgical consultation for severe or progressive deficits.
Trusted Resources to Go Deeper
- Comprehensive overview: Cleveland Clinic on spinal stenosis
- Diagnosis and treatments: Mayo Clinic: diagnosis and treatment
- Patient-friendly primer: American College of Rheumatology: Spinal Stenosis
- Symptom explainer: Brown Health: Symptoms and Treatment
- Options round-up: Nine spinal stenosis treatment options
With the right combination of decompression strategies, progressive strengthening, and smart pacing, most people reclaim comfortable walking and everyday function. Relief is realistic—and it often starts with small, consistent steps this week.


